 A study on blood pressure ended early after researchers noticed a “huge difference in cardiovascular disease events” between groups, said Dr. Holly Kramer, a nephrologist and associate professor of medicine and public health sciences at Loyola University Medical Center. (jasleen_kaur / Flickr)
A study on blood pressure ended early after researchers noticed a “huge difference in cardiovascular disease events” between groups, said Dr. Holly Kramer, a nephrologist and associate professor of medicine and public health sciences at Loyola University Medical Center. (jasleen_kaur / Flickr)
One in three adults in the U.S. has high blood pressure, according to the Centers for Disease Control and Prevention. But nearly 107,500 lives could be saved in the country each year if a more intensive approach to lowering high blood pressure was implemented, a recent study asserts.
Led by the National Institutes of Health, researchers involved in the study evaluated the potential benefits a more intensive management of high blood pressure would have on adults ages 50 and older. Instead of aiming to keep systolic blood pressure below 140 mm Hg, as the current guidelines recommend, the Systolic Blood Pressure Intervention Trial aimed for 120 mm Hg.
Blood pressure is recorded by two numbers and written as a ratio. Systolic blood pressure, the top number, “measures the pressure in the arteries when the heart beats,” the American Heart Association states on its website. Diastolic blood pressure is the bottom number and “measures the pressure in the arteries between heartbeats.”
Normal blood pressure, according to the AHA, is 120/80 or lower, which reads as 120 over 80 millimeters of mercury. Dr. Holly Kramer, a nephrologist and associate professor of medicine and public health sciences at Loyola University Medical Center, is the lead author of the study. She says optimal blood pressure is in the range of 115 to 120. “Meaning the blood pressure we normally have in our 20s,” she said.
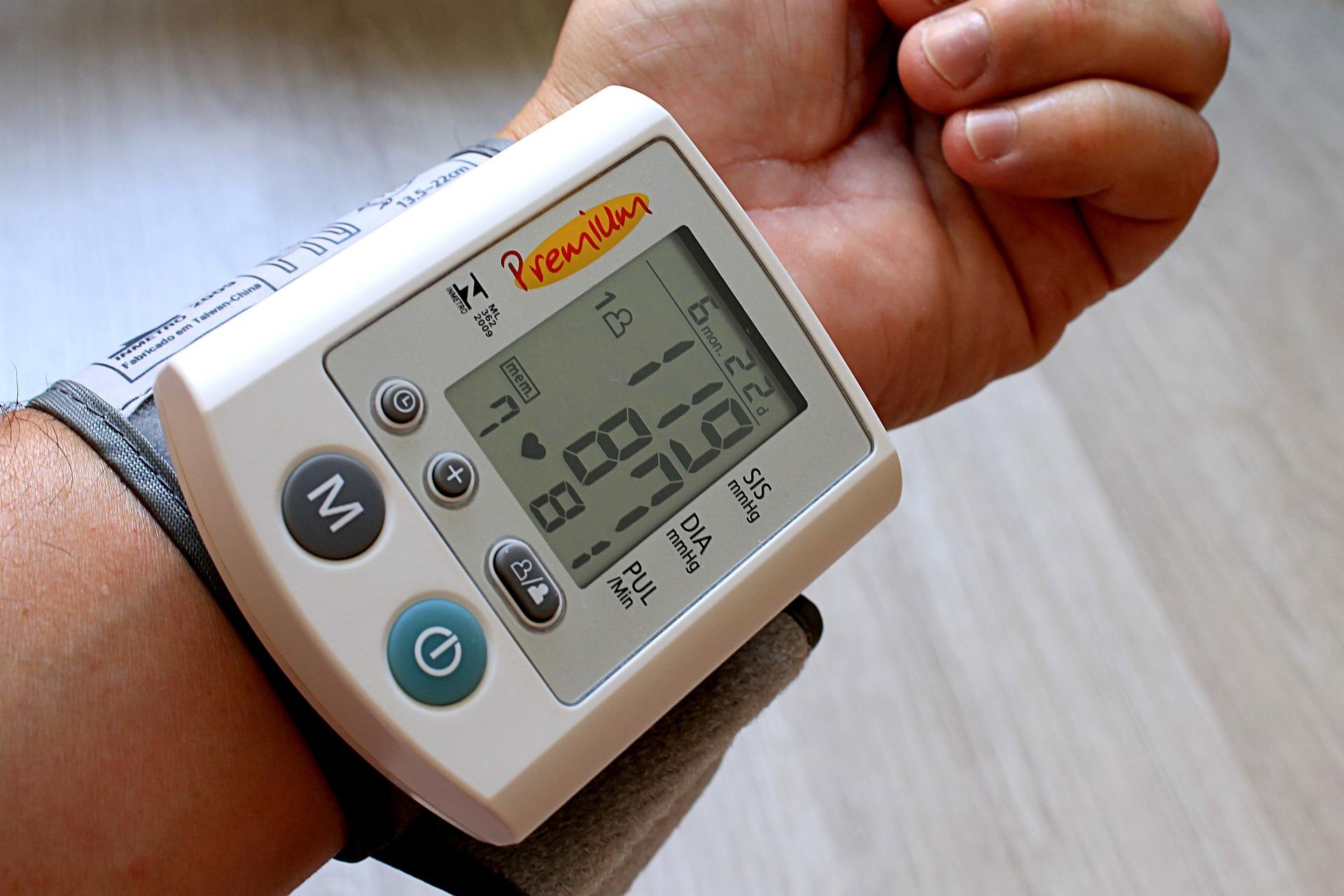 Dr. Holly Kramer recommends people interested in starting an intensive systolic blood pressure lowering program speak with their doctors and “weigh the risks and the benefits.” (Pixabay)
Dr. Holly Kramer recommends people interested in starting an intensive systolic blood pressure lowering program speak with their doctors and “weigh the risks and the benefits.” (Pixabay)
Doctors can treat the condition, also called hypertension, with medication and lifestyle changes, said Kramer. But it “is one of the leading causes of cardiovascular disease, heart disease, peripheral arterial disease and stroke,” she said.
More than 9,350 adults ages 50 and older who had high blood pressure and were at risk of cardiovascular disease were enrolled in the five-year trial. (Certain patients were excluded from the study, including smokers and those who had diabetes or a history of stroke.)
Participants were treated with readily available blood pressure medications to lower their systolic blood pressure. They were randomly selected to have their blood pressure either lowered below 120 mm Hg (the treatment group) or 140 mm Hg (the control group).
“After 3.26 years, we stopped the study prematurely because it was such a huge difference in cardiovascular disease events,” between the groups, Kramer said. Deaths were 27 percent lower in the group that had gotten more intensive treatment, she said.
Researchers applied those findings to the estimated 18.1 million American adults who met the study’s criteria and found that more than 107,500 deaths could be prevented each year if such an approach was taken.
While Kramer was “pleasantly surprised” by the results, she says they would come with an increased risk of certain side effects, such as low blood pressure and fainting. “But I think if you have a physician follow them closely, these can be managed,” she said.
Once the trial ended, Kramer said a patient who was in the control group approached her to ask about starting an intensive systolic blood pressure lowering program. Kramer recommends others who are interested in starting such a treatment program speak with their physicians.
“Weigh the risks and the benefits,” she said. Additional medications and more frequent check ups with physicians may be required. “There are risks that come with it. If patients understood these excess risks that are associated with it, we can extend lifespans even in frail and elderly patients who may be willing to do it.”
The results of the study were presented Sept. 15 at the American Heart Association’s Council on Hypertension 2016 Scientific Sessions. The study has been submitted for publication.
Follow Kristen Thometz on Twitter: @kristenthometz
Related stories:
 Heated Marital Spats Linked to Heart Problems
Heated Marital Spats Linked to Heart Problems
June 6: Flying off the handle during a marital spat cannot only escalate the argument, but also increase a person’s risk of developing cardiovascular conditions, like high blood pressure, a new study says.
 Study on Aging Challenges Common Perceptions of What ‘Healthy’ Means
Study on Aging Challenges Common Perceptions of What ‘Healthy’ Means
May 23: By most medical standards, being healthy means you’re not battling a major disease like cancer, diabetes or cardiovascular disease. But a new study from the University of Chicago questions this traditional method of measuring health.
 Loyola University Offers Medical Students Meditation to Combat Stress
Loyola University Offers Medical Students Meditation to Combat Stress
Feb. 25: Why Loyola Medical students are being encouraged to learn Transcendental Meditation – and how it could make them better doctors.








